Catheter Insertion and Care
Postoperative Management
Preoperative Management
Review the recommended actions and processes for your facility and patient prior to the catheter insertion procedure.
Perioperative and Intraoperative Management
Explore more on the percutaneous PD catheter insertion technique.
Postoperative Management
Recap on the post-procedure activities associated with preparing your patient for discharge after PD catheter insertion.
Catheter Insertion and Care - Postoperative Management
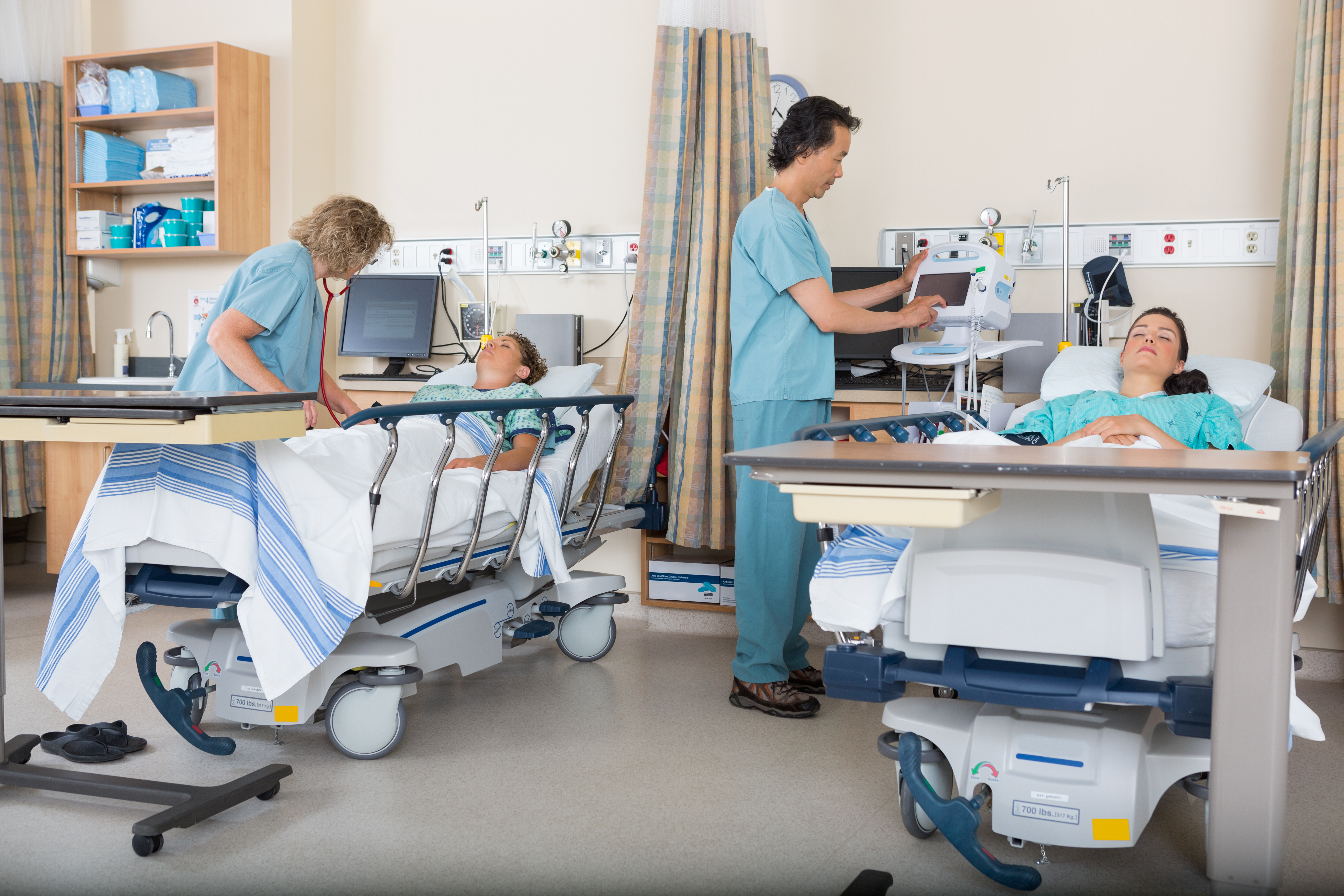
- Postoperative care includes
- Immobilization of the catheter to prevent exit-site and cuff trauma.
- Minimizing bacteria exposure and colonization.1
- Implantation should be timed to allow two weeks for healing prior to the initiation of dialysis.2
- Postoperative assessment and dressing should be changed weekly by experienced PD nursing staff only using aseptic technique with mask and gloves until healed.2
PD: Peritoneal Dialysis
Key Assessments

Assess exit-site and surgical wound for
- Bleeding, drainage, or leakage.
- Pain or tenderness on palpation.
Key Activities
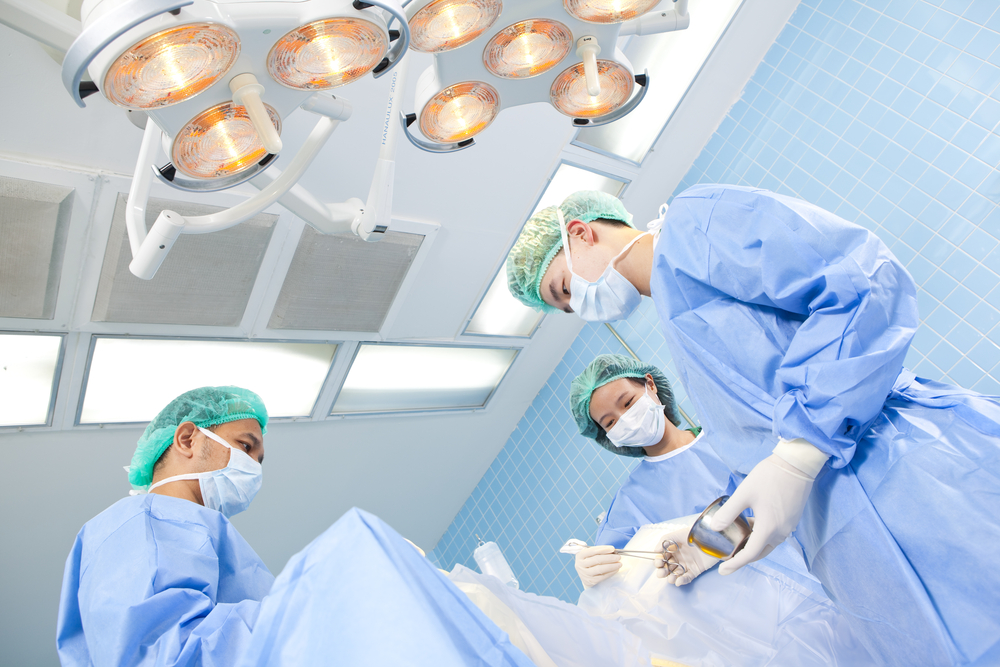
- Apply a non-occlusive gauze surgical dressing to immobilize the catheter, absorb drainage, and prevent trauma and contamination of the exit site.3
- Surgical or exit-site dressing should not be changed for five to ten days unless there is obvious bleeding or signs of infection.1,4
- Clean with nonirritating solution (i.e, nonionic surfactant, normal saline, or chlorhexidine).1,5
- Perform post-operative catheter flushing with dialysate or saline solution where necessary as per hospital protocol.3
Patient Education

- Maintain clean and dry dressing to protect from gross contamination and wetness.2
- Immobilize catheter.2
- Practice meticulous hand hygiene.6
- Avoid shower or bath until healed.1,5
- Limit strenuous physical activities, including heavy lifting, to minimize the risk of peritoneal leaks.3
- Notify PD unit in case of blood or other drainage, pain or tenderness, trauma to abdomen.
- Restrict dressing changes following implantation to experienced PD registered nurse.3
- Return to clinic for follow up as instructed by the PD nurse.